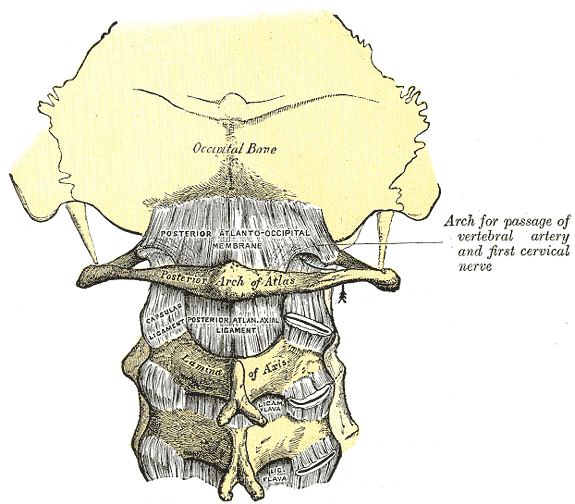
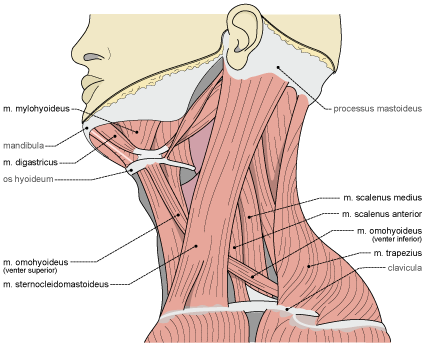
Rock Climbing Neck Injuries with Wil Seto
Mark: Hi, it’s Mark from TLR. I’m here with Wil Seto he’s the owner of the chief cook and bottle washer. Not really. He’s the big chief at Insync Physiotherapy in Vancouver and North Burnaby. And we’re going to talk about rock climbing neck injuries today. How are you doing Wil? Wil: I’m doing well….